|
8/10/2023 0 Comments Scar in eye retina 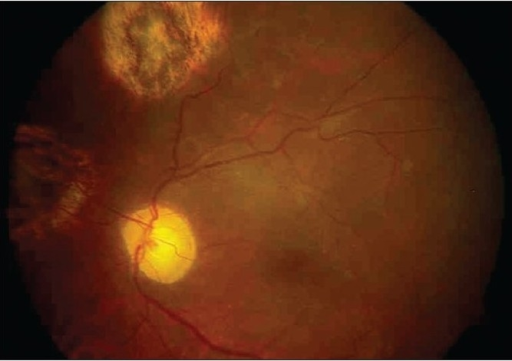
The advent of PCR-based diagnostics has greatly improved our ability to distinguish between toxoplasma and viral causes to necrotizing retinitis. Half the patients were initially treated as ARN prior to definitive diagnosis. reported 22 patients with widespread chorioretinitis from toxoplasmosis, including some with retinal vasculitis. Severe toxoplasma chorioretinitis can be mistaken for ARN, even absent a pigmented chorioretinal scar. He was continued on oral valacyclovir and prednisone postoperatively, with an attached retina and best-corrected visual acuity of 20/80 +1 five weeks after surgery. Since foscarnet does not need activation, brief incubation is thought to be sufficient for viral inactivation. Prior to fluid-air exchange and silicone oil injection, a standard 2.4 mg/0.1 mL dose of foscarnet was injected into the balanced salt solution-filled vitreous cavity and incubated for 5 min before washout. The patient underwent perfluorooctane-assisted 25-gauge pars plana vitrectomy with temporal retinectomy, extensive 360° endolaser, and intraocular tamponade with silicone oil. The day after his fourth foscarnet injection (14 days after symptom onset), the patient presented with a large retinal tear and focal RD in the area of temporal necrosis (shown in Fig. Due to worsening vitritis and stable to improving retinal whitening, he was started on 30 mg of oral prednisone daily 8 days after his initial foscarnet injection. He received intravitreal foscarnet injections every 3 days for a period of 10 days. We review emerging evidence for pigmented chorioretinal scars in ARN specifically caused by HSV-2, as well as diagnostic and treatment dilemmas in the management of ARN and ARN detachments.ĭue to the positive PCR results for HSV-2, trimethoprim-sulfamethoxazole was stopped, and the patient was continued on valacyclovir. The patient’s clinical course was complicated by rhegmatogenous retinal detachment within 2 weeks after symptom onset, requiring pars plana vitrectomy with silicone oil and intraoperative intraocular incubation with foscarnet. Management consisted of a dual therapy regimen of both oral and intravitreal antiviral agents as well as oral corticosteroids. The patient was treated for both ARN and toxoplasma chorioretinitis until PCR study of the vitreous and AC returned positive for HSV-2 and negative for toxoplasmosis. A superior pigmented chorioretinal scar with overlying contracted vitreous was noted in the periphery with no adjacent retinal whitening. An exam demonstrated anterior chamber (AC) reaction, vitritis, multifocal patches of whitening, and an occlusive retinal vasculitis. 
A 53-year-old functionally monocular male presented with painless floaters and blurry vision in his seeing eye over a period of 4 days. We report a finding of a pigmented chorioretinal scar with acute retinal necrosis (ARN) caused by herpes simplex virus 2 (HSV-2) infection rather than toxoplasma, creating an initial diagnostic dilemma. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
